Ashraf Engineer
May 15, 2021
PODCAST TRANSCRIPT
Hello and welcome to All Indians Matter. I am Ashraf Engineer.
As if the second wave of COVID-19 wasn’t bad enough, many states are reporting cases of mucormycosis, commonly known as the ‘black fungus’. The rare but potentially fatal infection is being found in COVID-19 patients with a number of cases detected in Maharashtra, Gujarat and Delhi. With well over 22 million COVID cases recorded so far and rising by more than 300,000 a day, this was the last thing India needed.
SIGNATURE TUNE
At the time of making this podcast, Maharashtra had at least 200 patients being treated for mucormycosis while eight had died of it. In neighbouring Gujarat, the state government created separate wards in hospitals for the treatment of the infection and ordered 5,000 doses of Amphotericin B, a medicine used to treat it. Infections were also reported in Delhi.
So, what exactly is mucormycosis and how does it affect the human body?
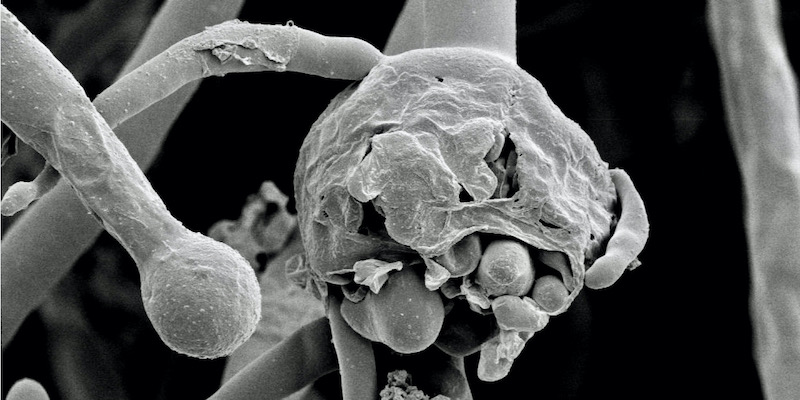
It’s a rare infection caused by moulds known as mucormycetes that occur naturally. It usually strikes those who are on medication for health problems that reduce their ability to fight pathogens in the environment. The moulds usually leave healthy persons unharmed.
Once such individuals inhale the mould spores, their sinuses and lungs are in danger. At this time, we are seeing a rise in such cases among COVID patients – so severe in some cases that they require urgent surgery.
The symptoms include pain and redness around the eyes or nose, dark nasal discharge with fever, headache, coughing, breathlessness, blood in the vomit and even an altered mental state. Other signs include cheekbone or jaw pain, skin lesions, blurry vision, thrombosis and chest pain.
Guarding against mucormycosis can’t be emphasised enough. It can lead to loss of the upper jaw and even the eye.
Here’s how can you prevent it.
If you have diabetes, are using steroids, have had a prolonged ICU stay and co-morbidities, you are vulnerable. Doctors have stressed the need to control diabetes, reduce steroid use and also to control hyperglycemia. COVID patients discharged after treatment should have their blood glucose level checked regularly.
Use masks if you are close to dusty areas – in fact, use masks anyway. Wear shoes, long trousers, long-sleeved shirts and gloves while handling soil, moss or manure.
So, what is the extent of the outbreak?
To be clear, while cases have been detected, it’s not a major outbreak.
However, it’s important to guard against it because, not only is mucormycosis devastating to health, the treatment can destroy you financially. One 50-milligram vial of the anti-fungal Amphotericin B costs Rs 8,000 and a minimum of 5 milligrams have to be given per kilogram of body weight. So, a patient weighing 50 kilograms needs 250 milligrams, which translates to Rs 40,000. Apart from this, patients need another anti-fungal, Posaconazole, the daily dose of which costs Rs 4,000.
The treatment also includes installing a peripherally inserted central catheter, maintaining systemic hydration, saline drips and monitoring through radio imaging.
The mucormycosis outbreak is only adding to India’s woes, and strangely it’s affecting young people a lot. Also, it’s not something expected in other countries. Experts have said that India’s high number of diabetics, combined with its unique climatic and environmental conditions, is what is helping mucormycosis thrive.
As always, prevention is the key. Mask up, stay inside and be extra vigilant if you have co-morbidities.
Thank you all for listening. Please visit allindiansmatter.in for more columns and audio podcasts. You can follow me on Twitter at @AshrafEngineer and @AllIndiansCount. Search for the All Indians Matter page on Facebook. On Instagram, the handle is @AllIndiansMatter. Email me at editor@www.allindiansmatter.in. Catch you again soon.